导图社区 How to against pathogens
- 23
- 0
- 0
- 举报
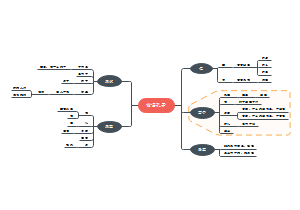
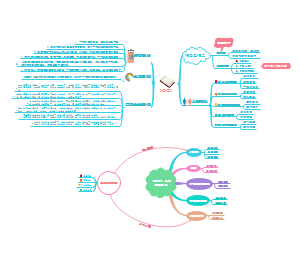
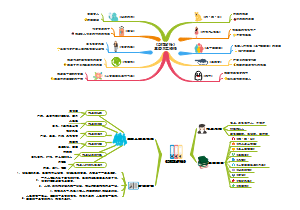
How to against pathogens
Inactivated toxin used in a vaccine. injected to stimulate the production of antitoxins and provide immunity.
编辑于2022-06-09 22:38:39- pathogens
- Vaccin
- antibiotics
- Drugs
- 相似推荐
- 大纲
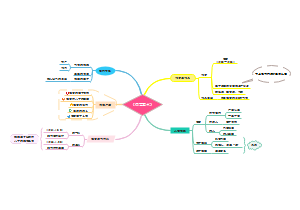
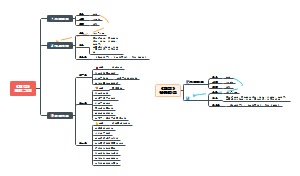
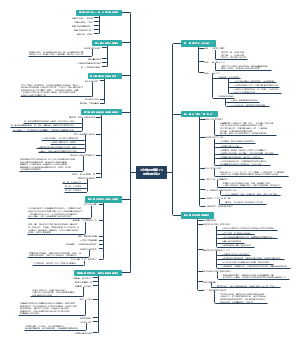
How to against pathogens
Vaccin
Dead antigens
treatment
inactivation
heat, formaldehyde or gamma irradiation
Recombinant
peptide
may discrete portion (domain) of a surface protein as Vaccine
each domains as an epitope
Subunit
benifits
Safe
Cheaper
both production and storage
weakness
number and specificity of antigen is usually not enough
They can't multiply
an antigen may not good enough as pathogen with full epitopes
also the antigen might be damaged
requires periotic boost
only stimulates partially B cells' clonal expansion
still have risk to contain un-Inactivated microbes
Cases
Toxoids
Inactivated toxin used in a vaccine. injected to stimulate the production of antitoxins and provide immunity.
antitoxin are antibodies against exotoxin
Vaccine can be made by inactivated exotoxin
heat, formalin or phenol
Inacivated virus
seed stock influenza virus in embryonic hens eggs
subcutaneous injection
Subunit(component) Vaccine
detergent treated then centrifuged envoloped viruses
ex. influenza virus
get rid of HA & NA
empty envolope
HBV
subcellular fragments
surface antigens
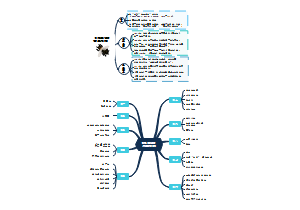
Live attenuated pathogens
Attenuation methods
lower the applied dose than infectious doses
grow pathogen in foreign host such as animals, embryonated eggs or tissue culture
Recombinat DNA
inserts genome of dangerous virus into genomes of some harmless virus (vector)
Safe for vector storage
less risk for damage, but higher cost to design
DNA vaccine
Ingect DNA genes for antigen along into muscle as vaccine
easy to design, prepare, storage and specific trageting
can elicit T cell immunity
risks for mutagenesis, allergy, and immunlogical tolerance
benifits
stimulates whole memorable adaptive immune response
including T cell immunity
inject one time in small amount, no needs for multiple booster.
orally possible
weakness
High risk, attenuation is easily reversed
risk for immunosuppressed individual
High cost for storage
Cases
Vaccina virus
ex.1
Insert HIV, rabies genome in nonessential region of harmless poxivirus
ex.2
Cold adapted (grown at 25ºC) influenza A & B
instranasal spray
10-15% NSTI (Necrotizing Soft Tissue Infection)
BCG (Bacillus Calmette Guerin vaccine for Mycobacterium tuberculosis)
Vector/DNA
Antiviral vaccines
Antibacteria vaccines
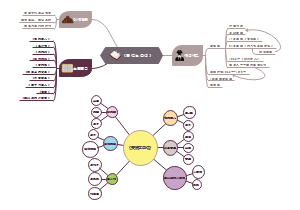
tricky definations
immunization
a procedure designed to increase concentrations of antibodies and/or effector T-cells which are reactive against infection (or cancer)
Vaccination
procedure of artificial active immunization
vaccine
agents of artificial active immunization
exeption
some times block fertilization
contraceptive vaccines
some times treat allergy
T cell vaccine
eliminate autoimmune T cells by using "bad T cells'" TCR as antigen ingection
benefit-to-risk ratio
benifits
lasting time of immunity
Qualitity
humoral and cellular activation
Cost
production
Storage
Application
risk
Autoimmunity/hypersensitivity
infection
Passive immunization
individual acquires immunity through the transfer of antibodies formed by an immune individual or animal.
via natural maternal serum/milk or artificial immune serum
not permenant, with out activation of clonal expansion, no memory cells
Active immunization
Immunization through providing antigen but not antibody
activates clonal expantion, permanent effect
may be artifatial or natural infection
Drugs
features
origin
natural
Synthetic
Semisynthetic
modified natural origin
most resent new antibiotics
range of effectiveness
Broad spectrum
Narrow spectrum
production
nature
synthesis
Half life
high half life ensure effectivness to target tissue
like coat should be stomach acid resistence
antiviral
Herpesvirals antivirals
viral DNA polymerase inhibitors
nucleoside analogue
acyclovir
Gancyclovir
cidofovir
pyrophosphate analogue
Foscarnet
Influenza antivirals
Amantidine (Rimantadine)
block M2 channel
M2 mutations develop resistence
Side effect: GI or CNS
Zanamivir (Relenza) and Oseltamivir (Tamiflu)
Neuraminidase Inhibitors
sialic acid analogous
18% resistence
for both type A&B
effect best in early stages
HIV antivirals
Entry Inhibitors
binds to macrophages' receptor CCR5
Fusion inhibitors:
Only one FDA-approved drug: fuzeon
RTIs: reverse transcriptase inhibitors
nucleoside-analogue RTIs (NRTIs)
non-nucleoside-analogue RTIs (NNRTIs)
distorts reverse transcriptase binding to RNA template
Integrase Inhibitors
PIs: protease inhibitors
HBV antivirals
Interferon
reverse transcriptase inhibitor
nucleoside analogue
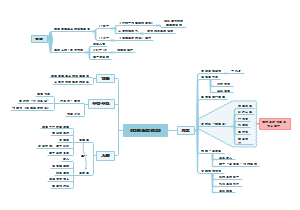
antibiotics
drops infectious desease motality from 0.797% to 0.036%
Antimicrobial susceptibility patterns
Bacteriostatic
Only inhibits growth but not kill bacteria
like inhibits protein synthesis
Bactericidal
kill bacteria but not lysis cell
Bacteriolytic
kill and lysis the cell
Antibiotic combinations
Reduce emergence of antibiotic resistance
results
Synergism
target different steps of route
Antagonism
ex bactericidal+bacteriostatic
QUNATIFY antibiotics' effects
Minimum Inhibitory Concentration (MIC)
observed growth reduction
Minimum Bactericidal Concentration (MBC)
Kills all, no recovery
Achieve selective toxicity
Target bacterial
Cell wall synthesis
β-Lactams inhibits transpeptidase which cross-links gram(+) peptidleglycan.
penicillin contains a β-lactams ring
most astonishing bacterial defense
producing enzyme β-lactamase
so use the enzymes inhibitor: e.x. potassium clavulanate to combine penicilin
Plasma membrane
effects selective permeability
ribosome
50s
30s
Streptomycin Causes Misreading of mRNA
transcription initiation
transcription elongation
Tetracyclin..
blocks incomming tRNA binds to A site
Erythromycin
blocks ribosome translocation
Resistance due to enzymatic methylation of 23S rRNA
DNA replication
gyrase
Ciprofloxacin
resistance due to mutations in the gyrase A subunit.
extremely broad ranged
Novobiocin
compete with ATP for binding to the B subunit of this enzyme and inhibit the ATP-dependent DNA supercoiling catalysed by gyrase.
resistance due to mutations in B subunit
RNA transcription
RNA pol
Rifampin
interferes with transcription initiation complex
fast resistence for mutations in RNA polymerase
so it self should not be used
metabolites
Tetrahydrofolate (THF) synthesis inhibitor
Sulfonamides
strucural analogous of paba
Trimethoprim
inhibits bacterial dihydrofolic acid reductase (DHFR; 105 greater effect on prokaryotic than eukaryotic enzyme)
Super bugs: microbes with multiple resistences
MRSA
Methicillin Resistant Staphylococcus aureus
Prevalence
Community acquired (CA) MRSA
Pandemic: 21-29% in adults and 35-50% in children
not multi-drug resistence
Healthcare associated (HA) MRSA
multi-frug resistence
Genetic elements
mec gene – staphylococcal chromosomal cassette (SCCmec)
5 types
MecA encodes PBP2a
alternative PBP(enzyme penicilin targets)
Resulting peptidoglycan is structurally different but functional.
B-lactamase genes can down regulates MecA gene transcripts
new antibiotics
•Linezolid •Quinupristin-dalfopristin •Daptomycin •Lysostaphin
VISA
Vancomycin intermediate susceptible strains
a little resistence to vancomycin
altered peptidoglycan biosynthesis which causes thicker cell walls and decreased drug exposure to the cytoplasmic membrane
VRSA
Vancomycin resistence strain
MIC>=32 ug/ml
Vancomycin binds terminal dipeptide in peptide side-chain and inhibits transglycosylation and transpeptidation
Vancomycin is unable to bind to its target site due to an altered terminal peptide.
Superbug-TB
Pathogen grows in macrophage and may become persistent
Thick lipid-rich outer membrane with mycolic acid limits uptake of antibiotics
Narrow porin channel transports b-lactams
against superbugs
Virulence genes target Antisense RNA
Develop New antibiotics
Use cocktails
Ristrict antibiotics use
track resistence data